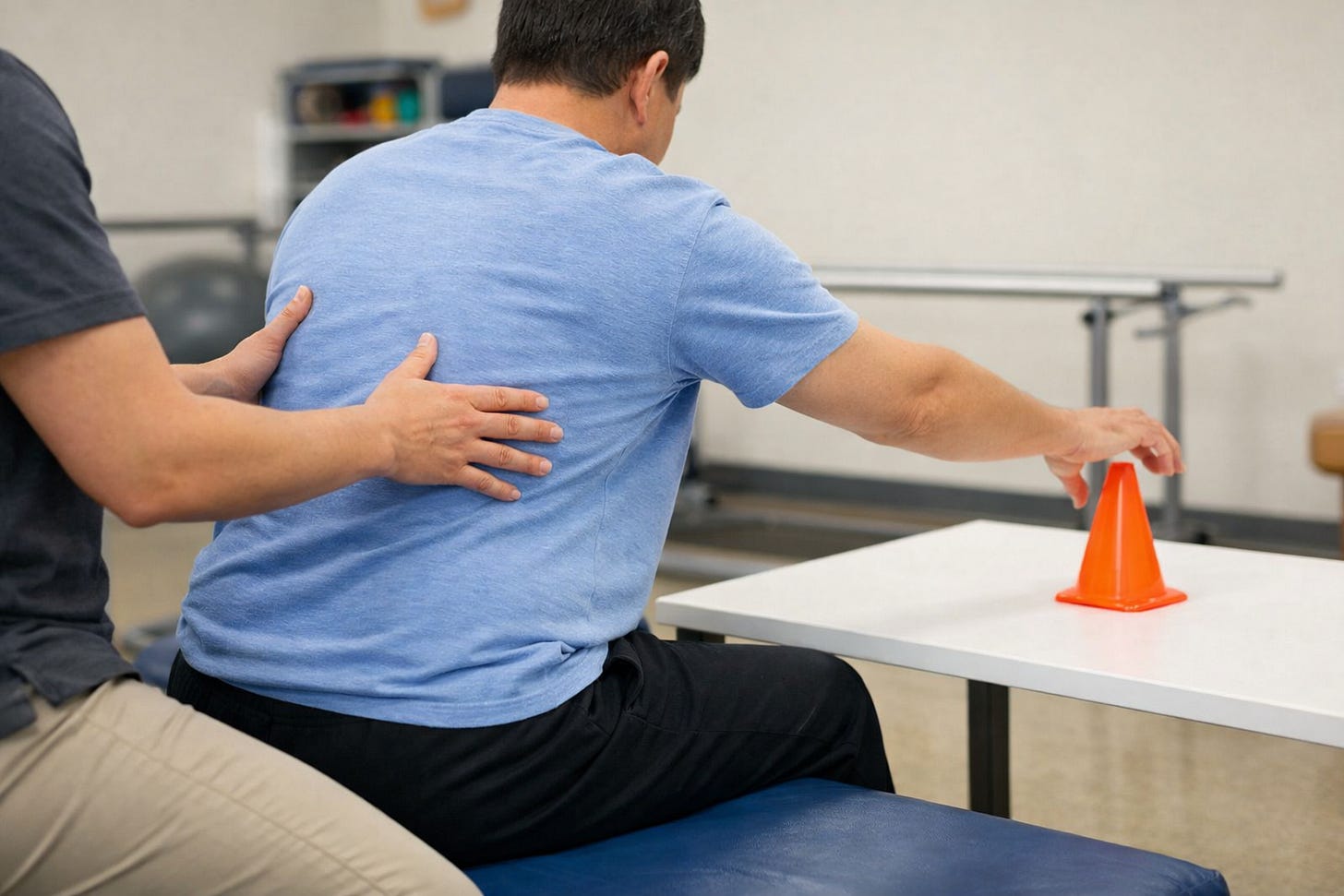
What Neuromuscular Re-Education Looks Like in Occupational Therapy
How movement patterns, balance, coordination, and posture are addressed in treatment to support everyday occupational performance.
In adult rehabilitation settings, range of motion and strength are often evaluated as part of the overall physical picture. These findings can suggest that a patient has the basic physical capacity to attempt a task. During functional activity, however, therapists may observe that the movement patterns used to complete the task are not well organized or coordinated.
A patient may have adequate shoulder range for grooming but cannot maintain upright posture long enough to complete the task. Another patient may have enough leg strength to stand but struggles to control the forward movement of the trunk that allows the body to rise from a seated position. A third patient may attempt to dress while sitting but loses midline alignment and repeatedly leans too far to one side.
In many of these situations, the primary challenge lies in how movement is organized during the task. The nervous system helps coordinate how different parts of the body move together during activity. For many everyday tasks, the trunk, hips, and limbs need to move in a coordinated sequence so the body can stay stable while movement occurs.
When that coordination is reduced, movement during tasks may appear less organized. The patient may lose balance when reaching, use more effort than expected during simple movements, or move in ways that look inefficient or unstable. Neuromuscular re-education addresses these kinds of movement patterns.
During treatment, the therapist structures activities that allow the patient to practice balance, coordinated weight shifting, and stable postural alignment while performing functional movements. These experiences give the nervous system opportunities to organize movement in a more consistent way. As movement patterns become more stable and coordinated, functional activities often become easier to perform. Tasks such as dressing, bathing, grooming, and transfers may begin to look smoother, more controlled, and more efficient.
Understanding the Core Focus of Neuromuscular Re-Education
Neuromuscular re-education often centers around several movement elements that show up repeatedly during functional activity. When therapists analyze how a task is performed, these elements often explain why a routine feels stable and efficient for one patient and difficult or effortful for another.
The four movement elements commonly addressed during neuromuscular re-education include:
Movement patterns – how different parts of the body work together during activity. Functional tasks require coordinated movement between the trunk, hips, shoulders, and extremities so the body can stay stable while the task unfolds.
Example: During lower body dressing, the patient rotates the trunk and reaches toward the feet while maintaining seated stability.Coordination – the timing and sequencing of movement. Many daily activities rely on movements happening in a particular order, such as shifting the trunk forward before standing or rotating slightly while reaching during dressing.
Example: During sit to stand, the patient shifts the trunk forward over the feet before pushing through the legs to rise.Balance – the ability to maintain stability while the body moves. Reaching, leaning, and turning during everyday tasks constantly shift the body’s center of mass, requiring the nervous system to make small adjustments to remain upright.
Example: While standing at the sink during grooming, the patient shifts weight between the lower extremities while reaching for items along the counter.Posture – the alignment and control of the body during activity. Stable postural alignment provides the foundation that allows the arms and legs to move efficiently during functional tasks.
Example: During seated bathing tasks, the patient maintains upright trunk alignment while reaching to wash different areas of the body.
These elements rarely appear alone. During everyday activities they are constantly interacting with one another. A dressing routine might involve trunk rotation, coordinated reaching, balance adjustments, and upright postural control all at the same time. When one of these elements becomes less organized, the entire task can become more difficult. Neuromuscular re-education focuses on helping the nervous system organize these elements more effectively so functional activity can unfold more smoothly.
Each of these elements contributes to the body’s ability to manage functional activity. When one area breaks down, the entire task can become inefficient or unsafe.
Recognizing Neuromuscular Re-Education During Treatment
Experienced therapists often recognize the need for neuromuscular re-education through careful observation of movement patterns during activity. When a patient performs a task, the therapist is not only looking at whether the task can be completed. They are also paying attention to how the body organizes movement throughout the activity. The quality of the movement often provides important clues about what may be limiting performance.
When movement appears poorly organized, inefficient, or unstable, neuromuscular re-education may be appropriate. These patterns often become visible during functional activities. A patient may technically complete a task, but the movement used to perform it may require excessive effort, appear unstable, or rely on compensatory strategies.
Common signs that neuromuscular re-education may be needed include:
Loss of trunk stability during reaching or task performance
The patient may lean excessively, brace with the arms, or collapse forward while attempting to reach or manipulate objects. Instead of maintaining a stable trunk while the arms move, the entire body shifts in a way that interrupts the task.Difficulty maintaining midline alignment
The patient may consistently lean to one side while seated or standing. Maintaining an upright position may require frequent corrections or external support. This can make tasks that involve reaching or sustained positioning more difficult.Uncoordinated weight shifting
Weight may not transfer smoothly between the lower extremities or across the base of support. The patient may hesitate before shifting weight, take multiple attempts to initiate movement, or rely heavily on the arms for stability.Poor balance during movement transitions
Movement between positions may appear unstable or abrupt. For example, the patient may struggle to maintain balance when turning, reaching, or lowering into a seated position.Inefficient movement sequencing during functional tasks
The order and timing of movement may appear disorganized. Movements that typically occur together may happen out of sequence, making the task appear effortful or slow.
Observations like these help guide treatment decisions. Rather than focusing only on strengthening individual muscles or repeating the task itself, the therapist may recognize that the underlying issue involves how the body is organizing movement.
In these situations, neuromuscular re-education provides a way to target the movement pattern directly. Structured activities can be used to help the patient experience more coordinated weight shifting, improved trunk stability, and more organized movement sequencing. Once these movement patterns become more stable and efficient, functional tasks often begin to feel easier and more predictable for the patient. This is why careful observation of movement during activity plays such an important role in identifying when neuromuscular re-education may be beneficial.
Why Functional Context Matters
Neuromuscular re-education is most effective when it connects to meaningful movement contexts. Functional activities naturally require the body to coordinate posture, balance, weight shifting, and movement sequencing. These activities create opportunities for the nervous system to experience how organized movement supports everyday performance.
When movement patterns are practiced in ways that relate to daily activity, the nervous system receives clearer feedback about how those movements are used in real life. Functional context strengthens carryover because the movement patterns being practiced are directly connected to daily routines.
In many sessions, this connection happens in two ways. First, functional tasks often reveal the movement patterns that need attention. As the patient performs dressing, bathing, grooming, or mobility activities, the therapist observes how the body organizes movement. Instability, inefficient weight shifting, or difficulty maintaining posture during the task may indicate a need for neuromuscular re-education.
Once these patterns are identified, the therapist may temporarily shift away from the task and introduce structured neuromuscular re-education activities that target the specific movement challenge. Practicing the movement outside of the task allows the patient to focus on trunk control, weight shifting, or movement coordination without the additional complexity of the full activity. After these patterns begin to improve, the patient returns to the functional task and applies the movement in context.
In other situations, elements of neuromuscular re-education can be integrated directly into task practice. The therapist may guide the patient to shift weight before reaching for an object, maintain trunk alignment while managing clothing, or control movement speed during transitions between positions. These adjustments allow the patient to experience more organized movement while still participating in the activity.
Targeted neuromuscular re-education outside of the task allows the movement pattern to be practiced in a focused way. Integrating the movement pattern back into functional activity helps the nervous system connect that movement to real life performance. This balance between movement practice and functional activity is one of the strengths of occupational therapy. It allows therapists to address the underlying organization of movement while keeping treatment closely connected to the activities that matter most in daily life.
Clinical Reasoning Behind Neuromuscular Re-Education
Selecting neuromuscular re-education as an intervention category reflects thoughtful clinical reasoning. The decision rarely begins with the intervention itself. It usually begins with careful observation of movement during functional activity. As the patient participates in tasks such as meal preparation, toileting, mobility, or other ADL tasks, the therapist watches how the body organizes movement throughout the activity.
The therapist is not only asking whether the patient can complete the task. They are asking how the movement unfolds during the task. Patterns that appear unstable, inefficient, or poorly coordinated often guide the decision to introduce neuromuscular re-education.
For example, during toilet hygiene a patient may struggle to rotate the trunk enough to reach behind the body. The patient repeatedly shifts the entire torso or loses balance while attempting the movement. The difficulty is not simply reaching. The challenge lies in coordinating trunk rotation while maintaining stable seated balance.
In this situation, the therapist may introduce neuromuscular re-education activities that focus on controlled trunk rotation and seated balance. The patient may practice rotating the trunk toward targets placed behind the body while maintaining stable positioning. These activities allow the nervous system to experience coordinated trunk rotation without the complexity of managing clothing or hygiene supplies.
Another example may occur during kitchen mobility. A patient standing at the counter may demonstrate difficulty turning to retrieve items placed behind them. The patient may take multiple small steps or pause before turning, indicating reduced coordination during directional changes.
In this case, the therapist may identify challenges with coordinated weight shifting and trunk rotation during turning movements. Neuromuscular re-education may then focus on structured standing rotation activities. The patient might practice controlled turning toward objects placed on different sides of the body while maintaining stable weight distribution through the lower extremities. As the patient experiences more organized rotational movement, turning during kitchen tasks often becomes smoother and more efficient.
A different pattern may appear during bed mobility. A patient attempting to move from supine to sitting may repeatedly struggle to coordinate trunk movement with lower extremity positioning. The movement may appear fragmented, with pauses or excessive effort during the transition.
Here, the therapist may identify difficulty coordinating movement sequencing between the trunk and lower body. Neuromuscular re-education might involve practicing partial rolling movements and trunk activation while transitioning through side-lying positions. These activities allow the patient to experience more coordinated movement patterns that support bed mobility. Once these patterns become more consistent, the patient may return to full bed mobility practice with improved movement organization.
Another example may occur during reaching tasks in a closet or storage area. A patient retrieving clothing from a shelf may demonstrate limited ability to reach upward while maintaining stable posture. The trunk may lean excessively backward or the patient may brace against nearby surfaces.
Neuromuscular re-education in this situation may involve practicing controlled overhead reaching in standing while maintaining stable trunk alignment and weight distribution. The therapist may structure reaching tasks at different heights so the patient can experience coordinated trunk stability while the arms move overhead. As these patterns improve, overhead reaching tasks become more controlled and efficient.
Across these situations, the clinical reasoning follows a consistent process. The therapist observes how movement patterns influence functional performance. Patterns that appear unstable or inefficient become targets for retraining. Treatment sessions then create opportunities for the nervous system to practice improved movement organization.
The therapist may adjust positioning, guide weight shifts, encourage trunk activation, or structure the environment so the patient experiences more stable movement patterns. Objects may be placed in positions that encourage rotation, reaching, or directional movement. Verbal or tactile cues may guide alignment and movement timing. Over time, these guided experiences allow the nervous system to refine how the body organizes movement. Functional performance often improves as movement becomes smoother, more coordinated, and more stable.
Bringing Neuromuscular Re-Education Into Everyday Practice
Once clinicians begin viewing treatment through the lens of movement organization, neuromuscular re-education becomes easier to recognize in everyday practice. Many familiar clinical observations lead directly to neuromuscular re-education interventions. A therapist may notice reduced trunk stability during dressing, inconsistent weight shifting during bathing preparation, loss of upright alignment while standing at the sink, or difficulty coordinating movement during transfers. These situations reveal movement patterns that are influencing occupational performance.
In many cases, neuromuscular re-education is introduced outside of the task itself so the movement pattern can be practiced in a more focused way. Practicing the movement separately allows the patient to concentrate on trunk control, balance, or coordinated weight shifting without the added complexity of managing clothing, hygiene tools, or environmental demands.
Other times, elements of neuromuscular re-education may also be incorporated during task practice. The therapist may guide a patient to shift weight before reaching, maintain trunk alignment while managing clothing, or control movement speed during a transition between positions. In these moments, the functional activity provides the context while the therapist helps shape how the movement occurs.
Both approaches work together during treatment. Targeted neuromuscular re-education outside of the task allows the movement pattern to develop in a controlled way. Practicing the task allows that movement pattern to be integrated into everyday activity. Through this process, neuromuscular re-education directly supports occupational performance. As movement patterns become more organized, everyday activities often begin to feel more stable, efficient, and predictable.
How Neuromuscular Re-Education Connects to ADL Performance
One of the reasons neuromuscular re-education can feel difficult to identify is that the movement issues it addresses often show up during everyday activities. Many occupational therapy sessions involve tasks such as dressing, bathing, grooming, or toileting. These activities naturally require the body to shift weight, maintain posture, rotate the trunk, and coordinate multiple movements at once. As the patient performs the task, the therapist is often paying close attention to how those movements are happening. ADL performance frequently reveals the movement patterns that need attention.
A patient may lose balance while reaching for clothing, lean excessively while washing the lower body, or collapse forward while sitting at the sink during grooming. In these moments, the therapist is not only observing whether the task can be completed. They are also analyzing how the body organizes movement throughout the activity. These observations often guide the next step in treatment.
While ADL training focuses on practicing the task itself, neuromuscular re-education addresses the movement patterns that are limiting performance. A dressing task may reveal reduced trunk stability while the patient reaches toward the feet. Instead of repeatedly attempting the dressing task with the same movement pattern, the therapist may shift the session toward targeted neuromuscular re-education activities that address trunk control and weight shifting in a more controlled environment.
The patient might practice seated reaching tasks, trunk rotation, or lateral weight shifting while maintaining upright alignment. These activities allow the patient to experience more organized movement patterns without the additional complexity of managing clothing. Later, the patient returns to the dressing task and applies those improved movement patterns during the activity. In this way, ADL performance and neuromuscular re-education often work together during treatment. The functional task helps reveal the movement challenge. Neuromuscular re-education provides a focused way to retrain the movement pattern. When the patient returns to the activity, the task often becomes more stable and efficient.
This process reflects a common rhythm in occupational therapy sessions. Functional activities reveal the movement challenges affecting performance. Neuromuscular re-education then targets those movement patterns in a structured way so they can better support everyday tasks. Over time, improvements in these movement patterns begin to support smoother and more efficient self-care performance.
Trunk Control to Support Dressing
Dressing tasks frequently place significant demands on trunk control. During lower body dressing, patients often lean forward to reach the feet, shift weight while threading clothing over the legs, or rotate the trunk to retrieve clothing from a nearby surface. These movements require the trunk to remain stable while the arms and legs move through the task. When trunk control is reduced, dressing may become slow, effortful, or unsafe.
A patient may repeatedly brace with the arms on the bed or chair, lean excessively to one side while reaching, or lose midline alignment when bending forward toward the feet. These patterns can interrupt the dressing routine and increase the risk of losing balance. When this type of movement pattern is observed during ADL performance, neuromuscular re-education may be introduced to address the underlying trunk control needed for the activity.
The therapist may guide structured trunk control activities in sitting that focus on maintaining upright alignment while performing controlled reaching, trunk rotation, or lateral weight shifting. The patient may practice reaching toward objects placed at different levels and angles while maintaining stable trunk alignment. These activities allow the patient to experience coordinated trunk movement without the additional complexity of managing clothing.
The goal is to help the nervous system develop more organized trunk control during reaching, rotation, and weight shifting. As trunk coordination and stability improve during these movement-based activities, those patterns often carry over when the patient returns to dressing tasks. Reaching toward the feet, retrieving clothing, and maintaining seated balance during clothing management can begin to feel more stable and efficient.
Example Daily Note
Objective: Patient participated in neuromuscular re-education targeting trunk stability and coordinated weight shifting in seated position to support lower body dressing performance. Therapist guided patient through structured trunk control activities including forward reaching toward targets placed near the feet, controlled trunk rotation toward objects positioned laterally, and lateral weight shifting while maintaining upright alignment over the pelvis. Patient initially demonstrated excessive lateral leaning and intermittent use of upper extremities for support during reaching tasks. With repeated practice and verbal cueing for trunk alignment, patient demonstrated improved ability to maintain midline stability while performing controlled reaching and rotation.
Assessment: Patient demonstrates reduced trunk stability and inconsistent weight shifting during seated reaching activities that influence lower body dressing performance. Neuromuscular re-education activities facilitated improved trunk organization and midline control during functional reaching patterns. Patient demonstrates emerging carryover of trunk alignment strategies that are expected to support improved stability during seated dressing tasks. Continued intervention will target coordinated trunk control and weight shifting to support safe and efficient lower body dressing.
Weight Shifting for Bathing
Bathing routines often require the body to shift weight while reaching, leaning, or changing positions. Patients may lean forward to wash the lower extremities, reach across the body to wash different areas, or shift weight while stepping into or out of a tub or shower. These movements rely on coordinated weight shifting and stable balance.
When coordinated weight shifting is reduced, bathing tasks may appear hesitant or inefficient. A patient may avoid reaching certain areas, move cautiously, or rely heavily on external supports to maintain stability. When this pattern is observed during bathing or bathing simulation, neuromuscular re-education may be introduced to address the underlying balance and weight shifting demands.
The therapist may guide structured standing activities that emphasize controlled lateral and forward weight shifting while maintaining stable trunk alignment. The patient may practice transferring weight between the lower extremities while reaching toward objects placed at different heights and positions. Practicing these movements in a simplified setting allows the patient to focus on coordinated weight shifting without the additional demands of managing bathing supplies or navigating wet surfaces. The goal is to help the nervous system develop more coordinated weight shifting and balance reactions during standing movement. As these patterns become more stable, patients often demonstrate improved confidence and control when returning to bathing tasks that require reaching, leaning, or stepping.
Example Daily Note
Objective: Patient participated in neuromuscular re-education targeting coordinated weight shifting and standing balance to support bathing-related reaching tasks. Therapist guided patient through structured standing activities including controlled lateral weight shifts between lower extremities and forward weight shifting while reaching toward objects positioned at varying heights and directions. Patient demonstrated hesitation with lateral weight shifting and increased reliance on upper extremity support during reaching tasks. With repeated trials and verbal cueing for trunk alignment and weight distribution, patient demonstrated improved ability to shift weight between lower extremities while maintaining upright stability.
Assessment: Patient demonstrates reduced coordination of weight shifting during standing movement patterns that influence stability during bathing-related reaching tasks. Neuromuscular re-education activities facilitated improved balance reactions and weight transfer during standing reaching activities. Patient demonstrates emerging ability to maintain stable trunk alignment during directional weight shifts. Continued intervention will target coordinated weight shifting and standing stability to support safe participation in bathing routines.
Postural Alignment to Support Grooming
Grooming routines often place sustained demands on postural control. Standing at the sink while brushing teeth, shaving, or styling hair requires the body to maintain upright alignment while the arms perform detailed movements for several minutes at a time.
When postural control is reduced, patients may rely heavily on the counter for support, distribute weight unevenly through the lower extremities, or gradually lose upright trunk alignment during the activity. These patterns often increase the physical effort required to complete grooming and can make it difficult to sustain the task. When these movement patterns are observed during grooming, neuromuscular re-education may be introduced to target the postural stability needed to support the activity.
The therapist may guide standing postural control activities that emphasize maintaining upright trunk alignment during reaching tasks at shoulder height. The patient may practice controlled reaching and subtle weight shifts while maintaining a stable stance as they interact with objects positioned at different heights and directions. Practicing these movements in a simplified setting allows the patient to focus on trunk stability and sustained upright alignment without the additional demands of managing grooming tools or hygiene routines. The goal is to help the nervous system organize postural control during standing movement. As stability improves, patients often demonstrate better endurance and alignment when returning to grooming tasks at the sink, allowing the activity to feel more efficient and less physically demanding.
Example Daily Note
Objective: Patient engaged in neuromuscular re-education targeting standing postural alignment and trunk stability to support grooming tasks performed at sink level. Therapist guided patient through structured standing activities emphasizing maintenance of upright trunk alignment while performing repeated reaching tasks at shoulder height and varying directions. Patient initially demonstrated forward trunk leaning and uneven weight distribution during reaching activities, requiring intermittent verbal cueing for postural correction. With repeated practice, patient demonstrated improved ability to maintain upright trunk alignment and consistent weight distribution through lower extremities while performing reaching movements.
Assessment: Patient demonstrates reduced postural stability during standing activities requiring sustained upright alignment, affecting tolerance for grooming tasks performed at sink. Neuromuscular re-education activities supported improved trunk alignment and postural control during standing reaching patterns. Patient demonstrates improved endurance for maintaining upright posture during functional standing activities. Continued intervention will target postural stability and standing tolerance to support grooming performance.
Controlled Movement to Support Transfer Descent
Transfers often require the body to control movement while lowering into a seated position. During sit to stand and return to sitting, the trunk and lower extremities must coordinate so the body lowers gradually into the chair. This movement requires controlled weight shifting, stable trunk alignment, and coordinated movement through the hips and knees.
When this coordination is reduced, the patient may descend quickly into the chair instead of lowering in a controlled way. This can involve heavy reliance on the arms, loss of trunk alignment, or abrupt contact with the seat. These patterns place additional stress on the joints and reduce overall movement safety. When this type of descent is observed during transfers, neuromuscular re-education may be introduced to address the movement control required for a more gradual, coordinated return to sitting.
The therapist may introduce targeted movement practice that emphasizes gradually lowering the body while maintaining trunk alignment and even weight through the lower extremities. The patient might practice lowering toward a raised surface from standing while focusing on controlled bending through the hips and knees. Practicing this component of the movement separately allows the patient to experience the timing and control needed for a smoother descent without managing the full transfer. The goal is to help the nervous system develop more consistent control during lowering transitions. As this control improves, patients often demonstrate a steadier and more coordinated return to sitting during transfers.
Example Daily Note
Objective: Patient participated in neuromuscular re-education targeting controlled lowering patterns and coordinated weight distribution through the lower extremities to support transfer safety. Therapist guided patient through structured standing activities emphasizing gradual lowering toward a raised surface while maintaining upright trunk alignment and symmetrical weight distribution. Patient performed repeated partial lowering movements focusing on controlled hip and knee flexion with consistent trunk alignment. Patient initially demonstrated rapid descent and increased reliance on upper extremity support. With repeated trials and verbal cueing for movement pacing and alignment, patient demonstrated improved ability to lower toward the surface with controlled movement and reduced reliance on arm support.
Assessment: Patient demonstrates reduced control during lowering movements associated with transfer tasks, resulting in abrupt descent patterns. Neuromuscular re-education activities supported improved coordination of trunk alignment and lower extremity movement during controlled lowering. Patient demonstrates emerging ability to regulate descent speed and maintain balanced weight distribution during movement transitions. Continued intervention will target controlled movement patterns and coordinated weight shifting to support safe transfer performance.
Seeing Neuromuscular Re-Education More Clearly
When clinicians begin looking for the movement patterns underneath functional tasks, neuromuscular re-education becomes easier to identify. The focus shifts from simply completing the task to understanding how the body organizes movement during the task. This perspective allows therapists to recognize when the nervous system needs support in developing more coordinated patterns.
It also clarifies why certain interventions belong within the neuromuscular re-education category. The goal is not simply activity completion. The goal is improving the way the body organizes movement so everyday activities become safer and more efficient. Once that distinction becomes clear, neuromuscular re-education begins to appear throughout many occupational therapy sessions.
A Final Thought
Neuromuscular re-education is not limited to specialized exercises or isolated techniques. In many treatment sessions, it develops through a combination of focused movement training and functional activity. Therapists often identify movement challenges while a patient is performing everyday tasks. The task reveals how the body is organizing movement and where stability, coordination, or balance may be breaking down. From there, neuromuscular re-education may be introduced outside of the activity so the patient can practice the movement pattern in a more structured way.
These focused movement experiences give the nervous system opportunities to organize balance, coordination, and postural control without the additional complexity of managing a full task. As those patterns begin to improve, the patient returns to the activity and applies the movement within the functional routine.
At times, elements of neuromuscular re-education may also occur within task practice. A therapist may guide a weight shift before reaching for an object, encourage trunk alignment while managing clothing, or cue controlled movement during a transition between positions. These moments allow the patient to experience the movement pattern within the activity itself.
Together, these approaches create a natural rhythm during treatment. Functional tasks reveal the movement patterns affecting performance. Neuromuscular re-education helps retrain those patterns. The activity then provides an opportunity to apply the movement within daily routines.
When therapists recognize these opportunities and guide them intentionally, neuromuscular re-education becomes a powerful tool for supporting occupational performance in adult rehabilitation.
If you enjoy learning how movement patterns connect to everyday occupational performance, the paid version of OT Practice Toolkit expands these ideas even further.
Paid posts include detailed intervention breakdowns, diagnosis specific examples, structured progression strategies, and documentation language banks that help translate clinical reasoning into clear, professional notes.
You can explore the paid subscription anytime if you would like deeper clinical guidance and practical tools for adult occupational therapy practice.